
The hard truth: a private MRI for chronic back pain is often a poor investment that finds clinically irrelevant issues, creates anxiety, and doesn’t change your treatment plan.
- The vast majority of “abnormalities” found on MRIs, like “degenerative disc disease,” are normal age-related changes and not the source of your pain.
- Its real value is to rule out rare but serious “red flag” conditions or to provide a map for a surgeon if you’re already a candidate for an operation.
Recommendation: Before paying for a scan, invest in a thorough assessment with a modern physiotherapist focused on function and movement, not just imaging. A scan should be the last step, not the first.
You’ve had back pain for months, maybe years. Your GP has been helpful, but the pain persists. An X-ray was done, and the report came back “normal” or showing only “minor wear and tear.” Yet, the pain is very real. Now you face a classic dilemma: wait weeks or months for an NHS referral, or take matters into your own hands and pay upwards of £300 for a private MRI. It feels like the logical next step, a way to finally get a definitive answer.
As a radiologist specialising in the spine, I see patients in this exact position every day. The belief is that the MRI machine is a magic box that will pinpoint the source of the pain and unlock the secret to a cure. But the clinical reality is far more nuanced. While MRIs are incredibly powerful for visualising soft tissues like spinal discs and nerves, their role in managing chronic, non-specific back pain is widely misunderstood. Often, the “answers” they provide are more confusing than helpful.
This guide isn’t here to tell you what to do, but to give you the framework a specialist uses to evaluate the real-world value of a lumbar spine MRI. We won’t just list what an MRI can find; we’ll focus on the most important question: will the findings actually change your treatment? We’ll explore why a “perfect” scan doesn’t mean your pain isn’t real, and why an “abnormal” scan doesn’t mean you’re broken. The goal is to help you decide if that £300 is a smart investment in your health, or a costly ticket to a world of unnecessary anxiety.
To help you make an informed decision, this article breaks down the key factors to consider, from the practical challenges of the scan itself to the clinical and financial realities of its results.
Summary: Should You Get an MRI for Chronic Back Pain if X-Rays Look Normal?
- What Are Your Options If You’re Claustrophobic But Need an MRI?
- Why Patients with Metal Implants Can’t Have MRI Safely?
- MRI for Soft Tissue vs CT for Bone: Which Scan for Your Fracture?
- The “Degenerative Discs” Finding on Lumbar MRI That Doesn’t Explain Your Pain
- How to Prepare for an MRI to Avoid 30-Minute Rescans?
- Traditional vs Modern Physio: Which Heals Back Pain 30% Faster?
- The “Out-of-Pocket” Costs That Private Insurance Doesn’t Cover
- Is Going Private Worth £300/Month When NHS Care Is Free?
What Are Your Options If You’re Claustrophobic But Need an MRI?
Before even debating the clinical need for an MRI, a very real and practical barrier for many is claustrophobia. The thought of lying in a narrow tube for 30-45 minutes can be more daunting than the pain itself. This is not uncommon; research suggests that up to 15% of patients scheduled for an MRI experience some level of claustrophobia. Fortunately, both technology and preparation techniques have evolved significantly to manage this.
The first step is to know your scanner options. Most modern MRI scanners are “wide-bore,” featuring a 70cm opening compared to the traditional 60cm. This extra 10cm makes a remarkable difference in the feeling of spaciousness. Some centres also offer “open” MRI systems, which are not a tube at all but open on the sides. While these can be excellent for severe claustrophobia, they often have lower magnetic field strength, which may compromise image quality for certain spinal issues. It’s a trade-off between comfort and diagnostic detail that you should discuss with your referring clinician and the imaging centre.
This image shows a modern wide-bore scanner, highlighting its more open and patient-friendly design.
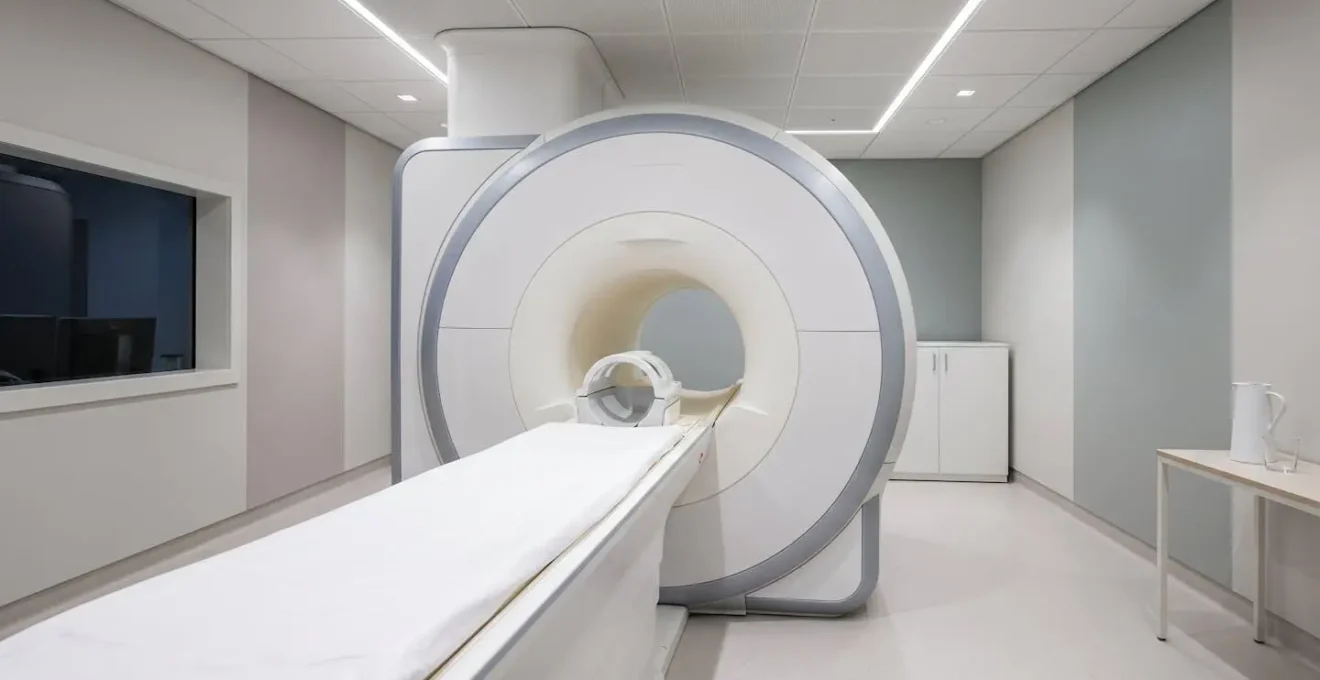
Beyond the hardware, preparation is key. You can proactively manage anxiety by communicating your fears early, discussing mild sedation options (like Diazepam) with your GP, and practicing stillness techniques at home. Many centres also provide headphones with music or podcasts, and a panic button is always within reach, giving you ultimate control. Acknowledging the fear and planning for it is the most effective strategy.
Why Patients with Metal Implants Can’t Have MRI Safely?
The powerful magnetic field used in MRI is the reason for strict safety protocols regarding metal in or on the body. The concern is twofold: the magnet can cause a metallic object to move or heat up, potentially causing injury. Secondly, the metal can create a large “artifact” on the images—a blacked-out or distorted area that can obscure the anatomy the radiologist needs to see, rendering the scan diagnostically useless.
However, the statement “can’t have MRI safely” is an oversimplification in the modern era. The critical factor is the type of metal. Ferromagnetic metals (like iron) are strongly attracted to the magnet and are generally ‘MR Unsafe’. But as the American College of Radiology points out, the landscape has changed significantly. In their manual on MR safety, they state:
Most modern implants are made from non-ferromagnetic substances and are labeled as MR-safe or MR-conditional.
– American College of Radiology, Manual on MR Safety: 2024 Update
This is crucial. An implant labeled ‘MR Safe‘ (e.g., made of titanium) poses no known hazards. One labeled ‘MR Conditional‘ means it is safe under specific conditions, such as a certain magnet strength (e.g., 1.5 Tesla but not 3 Tesla). This is why having your exact implant information is non-negotiable. Before even scheduling an MRI, you must inform both your doctor and the imaging center about any implants, including spinal fusion hardware, artificial joints, pacemakers, or even surgical clips. The radiology department will have a protocol to verify the device’s safety status, often by using your implant card or contacting the manufacturer. Never assume an implant is unsafe; always verify.
MRI for Soft Tissue vs CT for Bone: Which Scan for Your Fracture?
Patients often wonder why they need an MRI when an X-ray or CT scan has already been done. The answer lies in what each imaging modality is designed to see. Think of it like this: a CT scan is the expert for bone, while an MRI is the expert for soft tissue. An X-ray is a basic scout image that is good at showing gross bone alignment and obvious fractures but provides very little detail on anything else.
For back pain, this distinction is critical. If your doctor suspects a subtle or complex fracture, a bony spur pressing on a nerve (osteophyte), or stress fractures from overuse (spondylolysis), a CT scan provides unparalleled bony detail. It creates a 3D map of your vertebrae and is far superior to MRI for characterising bone structure. However, it uses ionising radiation (though modern doses are very low) and is poor at visualising the discs, spinal cord, and nerves themselves.
An MRI, on the other hand, uses no radiation. Its superpower is its exquisite detail of soft tissues. It is the only modality that can directly visualise a herniated disc, show the extent of nerve root compression, evaluate the spinal cord for any abnormalities, and assess the hydration (and therefore health) of the discs. For the vast majority of back pain investigations where the concern is a “slipped disc” or sciatica, MRI is the tool of choice. The table below, based on data from diagnostic imaging specialists, summarises the key differences.
This comparative analysis helps clarify which scan is appropriate for different diagnostic questions, with the information compiled from a recent overview of imaging for back pain.
| Imaging Type | Best For | Radiation | Key Advantage | Limitation |
|---|---|---|---|---|
| MRI | Soft tissue: spinal cord, nerves, herniated discs, disc degeneration | None | Most effective for soft tissue visualization and nerve compression | Limited bone detail; not ideal for subtle fractures |
| CT Scan | Bone structure: fractures, bony spurs (osteophytes), stress fractures (spondylolysis) | Yes (low dose) | Superior bone imaging; detects fractures MRI may miss | Poor soft tissue detail compared to MRI |
| Bone Scan (Scintigraphy) | Functional imaging: detects areas of high bone turnover, inflammation, tiny fractures, arthritis | Yes (radiotracer) | Locates ‘hot spots’ of bone activity when source of pain is mysterious | Low anatomical detail; requires follow-up imaging |
The “Degenerative Discs” Finding on Lumbar MRI That Doesn’t Explain Your Pain
This is arguably the most important concept for any patient with chronic back pain to understand. You get your £300 MRI, and the report comes back with a list of intimidating terms: “degenerative disc disease,” “disc bulge,” “desiccated discs,” “facet arthropathy.” It sounds alarming and seems to be the clear cause of your pain. But from a clinical standpoint, these findings are often meaningless.
The crucial point is that these changes are an incredibly common and normal part of the aging process. They are the spinal equivalent of getting gray hair or wrinkles on your skin. They are not a “disease” but a description of age-related wear. The evidence for this is overwhelming. Multiple large-scale studies have performed MRIs on thousands of people with absolutely no back pain, and the results are stunning. Landmark research published in the American Journal of Neuroradiology shows that disc degeneration is present in 37% of pain-free 20-year-olds, rising to 80% of 50-year-olds and 96% of 80-year-olds. In fact, up to 90% of healthy individuals over age 60 have findings of bulging discs on MRI without any associated pain.
This phenomenon is called the “pain-imaging mismatch.” The presence of a finding on a scan does not prove it is the cause of the pain. This is why getting an MRI “just to see what’s there” can be so counterproductive. It can provide you with a scary-sounding label that creates fear and anxiety, leading you to guard your back, avoid movement, and spiral into a cycle of chronic pain—all based on a finding that is likely irrelevant.
The real job of a clinician is to correlate the imaging findings with your specific physical symptoms. A small disc bulge is meaningless. A large disc bulge that is clearly pressing on the exact nerve that corresponds to your leg pain? That’s a significant finding. But more often than not, the MRI report is just a list of the spine’s natural, and beautiful, aging process.

How to Prepare for an MRI to Avoid 30-Minute Rescans?
An MRI scan’s quality is exquisitely sensitive to motion. Even tiny movements like coughing, fidgeting, or shivering can create artifacts that blur the images, making them undiagnosable. When this happens, the technologist has to repeat that portion of the scan, extending your time in the machine and increasing your anxiety. A 30-minute scan can easily turn into a 45- or 60-minute ordeal. Preparing for stillness is one of the most effective things you can do to ensure a smooth, efficient, and high-quality scan.
This preparation starts at home, well before your appointment. You can train your body and mind to lie still by practicing. A few days before the scan, try lying flat on your back on the floor, without a pillow, for 10-15 minute intervals. Put on some music or a podcast—just as you might in the scanner—and focus on staying completely motionless. This builds both physical and mental tolerance for the experience.
On the day of the scan, set yourself up for success. Wear comfortable, metal-free clothing (sweatpants and a t-shirt are ideal) so you don’t have to change. Avoid caffeine for several hours beforehand, as it can make you feel jittery and restless. When you arrive, communicate with the technologist. Let them know if you’re nervous or tend to feel cold. They can provide a blanket to prevent shivering (a major cause of motion artifact) and give you a heads-up before the longest, most critical imaging sequences so you can focus your efforts on being extra still during those key minutes.
Your Action Plan: Pre-Scan Preparation for a Motion-Free MRI
- At home training (1-2 weeks before): Practice lying still on the floor for 10-15 minute intervals while listening to music or a podcast to train your body and mind for the scan duration.
- Day before scan: Avoid caffeine after noon to reduce nervous energy and potential movement from restlessness.
- Arrival preparation: Wear comfortable, loose-fitting clothing without any metal components (zippers, snaps, underwire bras, metal buttons).
- During scan: Request a blanket from the technologist to stay warm (shivering causes movement), and ask for the imaging center’s music options or bring your own playlist.
- Communication strategy: Tell the technologist “I’m a bit nervous about staying still. Could you give me a heads-up before the longest sequences so I can specially prepare?” This turns them into your ally.
Traditional vs Modern Physio: Which Heals Back Pain 30% Faster?
The relentless pursuit of a diagnosis on an MRI is often driven by the belief that treatment cannot begin until the “problem” is found. However, modern approaches to back pain rehabilitation have turned this idea on its head. The evidence now strongly suggests that for the vast majority of chronic non-specific back pain, the most effective treatment is not based on a scan finding, but on restoring function and confidence in movement.
This marks a significant shift from “traditional” physiotherapy, which often relied on passive modalities. You might remember treatments involving heat packs, ultrasound machines, and gentle massage. While these can feel good temporarily, they do very little to address the underlying issues of deconditioning, fear of movement (kinesiophobia), and a nervous system on high alert. Modern, evidence-based physiotherapy is an active process focused on what you can do, not what your scan says.
This approach combines two powerful elements:
- Pain Neuroscience Education: Helping you understand that pain is a protective mechanism from the brain, not an accurate measure of tissue damage. This decouples the sensation of pain from the fear of harm, which is a critical step in recovery.
- Graded Exposure and Movement: A therapist works with you to identify movements you fear (like bending or lifting) and gradually re-introduces them in a safe, controlled way. This retrains the brain to understand that these movements are not dangerous, restoring your strength, mobility, and confidence.
Case Study: Active vs. Passive Physiotherapy
This modern, multidisciplinary approach is shown to be highly effective. A 2024 Bayesian network meta-analysis published in Scientific Reports compared various physiotherapeutic methods for chronic low back pain. The study concluded that a multidisciplinary program combining manual therapy, adapted physical exercise, education, and cognitive re-education was the most effective treatment for reducing disability. This active approach significantly outperformed passive modalities like heat and ultrasound in both pain reduction and, more importantly, long-term functional improvement.
The “Out-of-Pocket” Costs That Private Insurance Doesn’t Cover
The advertised price of a private MRI, around £300-£400, can seem like a straightforward, one-time expense for a quick answer. However, in the world of private healthcare, this initial figure is often just the beginning. The true “out-of-pocket” cost of going down the private imaging route can be significantly higher, a fact that catches many patients by surprise.
First, you need a referral from a specialist to get the MRI. This initial consultation with a private spinal surgeon or pain specialist can cost between £150 and £300. After the scan, you will need a follow-up consultation to discuss the results, which is another £150-£300. Suddenly, your £300 scan has become a £600-£900 investigation before any treatment has even begun.
Furthermore, one of the biggest hidden costs is the “diagnostic cascade.” An MRI is so sensitive that it often picks up incidental findings—abnormalities that are unrelated to your back pain, such as a simple cyst on a kidney or a benign lesion on the liver, which happen to be in the field of view. While the vast majority of these are harmless, once found, they often trigger a recommendation for further investigation “just to be safe.” This might mean a follow-up ultrasound (£200-£400) or a CT scan (£400-£600), creating more anxiety and more cost, all stemming from a scan that was meant to solve a different problem.
Before you commit, it’s vital to map out all potential expenses. Here are the key questions to consider:
- Consultation Fees: What are the costs for the initial referral and the follow-up results appointments?
- Scan Cost: What is the final, all-inclusive price for the MRI itself? Does it include the radiologist’s report?
- Cascade Costs: Have you budgeted for the possibility of needing further tests based on incidental findings?
- Insurance Details: If you have private insurance, what is your policy excess? Is pre-authorisation required? What is your co-insurance percentage for advanced imaging?
Key takeaways
- An MRI’s primary role in chronic pain is to rule out rare “red flags,” not to be a pain-finding tool.
- “Degenerative disc disease” and “disc bulges” are normal aging processes found in most pain-free adults and are rarely the source of your pain.
- The most effective path to recovery is often active physiotherapy focused on movement and function, which doesn’t require an MRI to begin.
Is Going Private Worth £300/Month When NHS Care Is Free?
We finally arrive at the ultimate strategic question. You understand the limitations of the scan, the potential for irrelevant findings, and the full scope of the costs. Is it still worth paying to bypass the NHS queue? The answer isn’t a simple yes or no; it’s a personal calculation of time, money, and peace of mind.
The core trade-off is clear: the NHS offers care that is free at the point of use but can involve significant waiting times, especially for non-urgent diagnostics. A wait of 6 to 18 weeks for a routine lumbar MRI is not uncommon. During this time, you may be living with pain, uncertainty, and potentially missing work. Private healthcare offers near-immediate access—often a scan within a week—but at a direct financial cost. For some, the cost of lost wages or diminished quality of life during the NHS wait is far greater than the cost of the scan itself.
However, the private route has its own pitfalls. The fee-for-service model can sometimes create an incentive for over-investigation. As we’ve discussed, this can lead to a cascade of further tests and costs. The NHS, for all its waiting times, provides a more integrated system that is generally better at managing complex conditions and is inherently cautious about unnecessary interventions. A specialist in the NHS is less likely to recommend a cascade of tests for a benign incidental finding. The table below outlines this strategic choice.
| Factor | Public Healthcare (NHS/Medicare) | Private Healthcare |
|---|---|---|
| Wait Time for MRI | 6-18 weeks for non-urgent cases | 1-7 days |
| Cost to Patient | Free at point of service (tax-funded) | £300-£800 per scan out-of-pocket |
| Choice of Specialist | Limited; assigned based on availability | Full choice of consultant and facility |
| Hidden Cost of Waiting | Potential lost wages, prolonged pain, decreased quality of life | Immediate financial outlay |
| Care Integration | Better-integrated care for complex conditions; no incentive for over-investigation | Faster access but potential for over-investigation due to fee-for-service model |
| Hybrid Strategy | Use public system for initial consultation, pay privately for MRI only (£400-£600), return to public system with results – optimizes time and cost | |
A sophisticated “hybrid” strategy is often the most pragmatic solution: stay within the NHS for your specialist consultation, but if an MRI is deemed necessary and the wait is long, pay privately for just the scan. You can then take the results back to your NHS specialist. This gives you the speed of the private sector for the diagnostic test while keeping you within the integrated, cost-free care of the public system for treatment planning.
The decision to get an MRI should be a calculated one, based on a clear clinical question. If your goal is to rule out a suspected serious condition or to plan for a surgery you’re already considering, it is an invaluable tool. If your goal is simply to find “the cause” of your chronic back pain, it’s more likely to be a costly and confusing detour. The most powerful next step is often not a scan, but a conversation with a skilled physiotherapist who can help you reclaim your movement and your life, regardless of what an image shows.