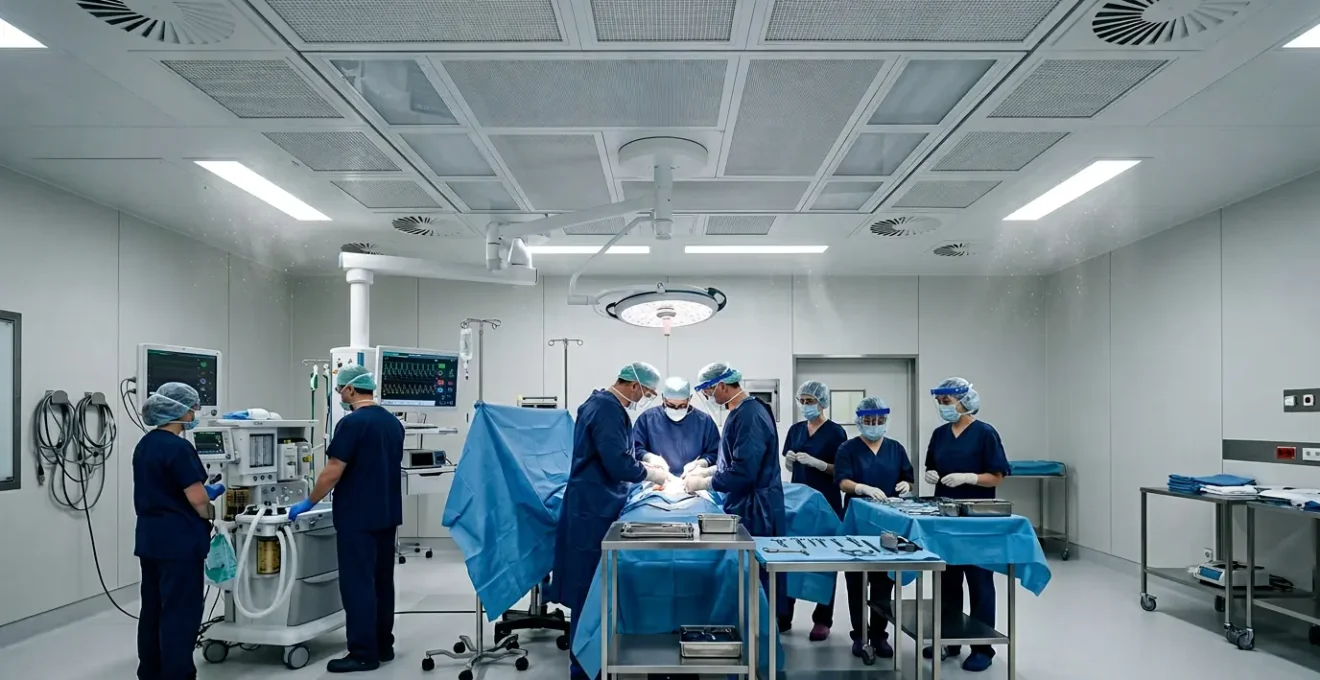
In summary:
- Preventing surgical infections like MRSA is not one single action but a chain of rigorously enforced, science-backed protocols.
- Your safety begins before you even enter the hospital, with specific pre-operative preparations designed to reduce bacteria on your skin.
- Inside the operating room, everything from the air you breathe to the instruments used is subject to validated sterility standards.
- Your role as an “active patient partner” in following pre- and post-operative instructions is a critical link in this safety chain.
- Every protocol is designed to break the chain of infection at a different point, creating multiple layers of defense.
The thought of undergoing a major operation, like a joint replacement or cardiac surgery, is daunting enough. But for many, the greatest fear isn’t the procedure itself, but the risk of acquiring a hospital ‘superbug’ like MRSA (Methicillin-resistant Staphylococcus aureus). You’ve heard the stories, and it’s natural to feel anxious. You’re often told that “staff wash their hands” and “you’ll get antibiotics,” but these reassurances can feel vague and insufficient when faced with the fear of a serious surgical site infection (SSI).
As an experienced operating theatre nurse, I want to pull back the curtain and show you what infection prevention truly looks like from our side. It’s far more than just surface cleaning. The real key to your safety lies in a philosophy of systematic, obsessive control. We see it as a “chain of infection,” and our mission is to break every single link in that chain through a series of interconnected, scientifically-validated protocols. This isn’t about hoping for the best; it’s about engineering a controlled environment where the risk of infection is driven to the absolute minimum.
This article will walk you through that chain of defense, step by step. We’ll explore why superbugs are a threat, how your own preparation is the first line of defense, what really happens to make an operating theatre safe, and why even the cost of surgical instruments is directly tied to your safety. Understanding this system will replace your fear with confidence in the process designed to protect you.
Summary: A Guide to Preventing MRSA in Surgery
- Why Do Standard Antibiotics No Longer Kill Hospital Superbugs?
- How to Shower with Hibiscrub Before Surgery to Reduce Risk?
- Laminar Flow vs. Standard Theatres: Which Is Safer for Joint Replacement?
- The Touching Mistake That Can Jeopardize a Fresh Surgical Wound
- When to Change Your Dressing: The 3 Signs of Early Infection
- The Ward Hygiene Mistake That Undermines a Perfect Operation
- Why Must “Sterile” Instruments Undergo 121°C Steam for 15 Minutes Specifically?
- Why Do Surgical Instruments Cost Thousands When Similar Tools Are So Cheap?
Why Do Standard Antibiotics No Longer Kill Hospital Superbugs?
To understand why we are so rigorous, we must first face the challenge: antimicrobial resistance. For decades, antibiotics were a magic bullet. But bacteria are incredibly adaptable. MRSA is a strain of a common bacterium, Staphylococcus aureus, that has evolved to survive the antibiotics we once relied on. It’s not that the antibiotics have changed; the bugs have. When you hear “superbug,” it simply means a microorganism that has built up defenses against multiple drugs, making infections much harder to treat.
The scale of this problem is significant. Globally, research from the Institute for Health Metrics and Evaluation revealed that more than 121,000 deaths in 2019 were directly attributable to MRSA antimicrobial resistance. This resistance is not a rare occurrence; it’s the new normal. For example, current epidemiological data shows that over 99% of clinical S. aureus strains are now resistant to penicillin, the original wonder drug. This is why a prophylactic (preventative) antibiotic given before your surgery is just one single layer of a much larger, more complex defense system. We can’t rely on it alone. The foundation of modern surgical safety is preventing the bacteria from ever reaching the surgical site in the first place.
How to Shower with Hibiscrub Before Surgery to Reduce Risk?
Your active participation in the safety protocol begins at home, typically the day before and the morning of your surgery. You’ll likely be instructed to shower with an antiseptic skin cleanser containing chlorhexidine gluconate (often known by the brand name Hibiscrub). This is far more than a simple wash. The goal is to drastically reduce the skin’s “bioburden”—the total number of bacteria present. While it’s impossible to sterilize skin, we can lower the bacterial count so significantly that the risk of them entering the wound is minimized.
The science behind chlorhexidine is what makes it so effective. It doesn’t just wash off. It chemically binds to the proteins in your skin, leaving behind a persistent antimicrobial barrier that continues to kill bacteria for hours after you’ve showered. This creates an invisible shield on your skin, providing an active defense right up until you enter the operating room. This process is highly optimized; a 2015 randomized prospective study demonstrated that following a standardized protocol achieves a maximal skin surface concentration of the antiseptic, ensuring the most effective barrier is formed.
As the illustration conceptually shows, this isn’t just surface-level cleaning; it’s about creating a lasting protective film. By following the showering instructions precisely, you become an active patient partner in the first crucial step of breaking the chain of infection. You are preparing the canvas for a safe surgical procedure.
Laminar Flow vs. Standard Theatres: Which Is Safer for Joint Replacement?
Inside the operating room (OR), we enter a completely controlled environment. One of the most discussed technologies is the laminar airflow system, which creates a curtain of ultra-clean, filtered air that flows directly over the surgical site to prevent airborne bacteria from settling into the wound. It seems logical that this would be universally safer. However, the reality is more nuanced and speaks to the core of our philosophy: it’s the entire system of disciplined protocols, not just one piece of equipment, that ensures safety.
Surprisingly, large-scale studies have challenged the assumption that laminar flow is always superior. For instance, a major analysis of six studies encompassing over 134,000 procedures found a slightly higher infection rate in theatres with laminar flow (0.6%) compared to those with conventional ventilation (0.5%) for joint replacements. This counter-intuitive finding is thought to be because the powerful airflow can create turbulence, potentially disrupting the sterile drapes or causing staff to move differently, which can be more disruptive than the air itself.
Case Study: The New Zealand Joint Registry Analysis
A landmark retrospective analysis of over 88,000 primary hip and knee replacements from the New Zealand Joint Registry found a statistically significant increase in deep infection rates in laminar flow theatres. This study challenged the industry’s long-held assumption, suggesting that factors like team discipline, minimizing movement and traffic in the OR, and meticulous sterile technique are likely more critical than the type of ventilation system used. It highlights that technology cannot replace rigorous human protocol.
The takeaway is not that technology is useless, but that it’s only one part of a complex system. The true defense is the disciplined choreography of the surgical team: minimizing chatter, restricting movement in and out of the OR, and maintaining an unwavering focus on the sterile field. This is the “controlled environment” in action.
The Touching Mistake That Can Jeopardize a Fresh Surgical Wound
After a successful operation, the “chain of infection” defense moves with you from the OR to the recovery ward. The surgical wound is now closed and covered by a sterile dressing, which acts as a physical barrier. While the overall risk of a surgical site infection (SSI) is relatively low— affecting 2% to 4% of patients undergoing inpatient surgery—vigilance during this phase is critical. The single most common and preventable mistake is allowing the sterile site to be touched unnecessarily, either by well-meaning relatives or even by healthcare staff who might have a momentary lapse in protocol.
Your wound is a gateway. Even after it is sealed, the surrounding skin and the dressing itself must be treated as a protected zone. Every touch introduces new bacteria and a new risk. This is where your role as an active patient partner becomes paramount. You are the final guardian of your wound. This doesn’t mean you should live in fear, but it does mean you are empowered to speak up to ensure the protocols are followed by everyone, including your care team and visitors.
Your Action Plan: Protecting Your Surgical Wound
- Hand Hygiene for All: Ensure all visitors wash their hands thoroughly before and after entering your room. Don’t be afraid to politely remind healthcare providers: “Would you mind washing your hands before checking my dressing?”
- Request Fresh Gloves: It is your right to ask staff to change their gloves before touching your surgical site. A simple, “Could you please use a new pair of gloves for this?” is perfectly acceptable and expected.
- Establish a No-Touch Boundary: Inform loved ones and friends that they must not touch the wound or the dressing, no matter how curious they are. Explain that this is a critical part of your recovery.
- Follow Instructions Meticulously: Adhere strictly to the wound care instructions given to you by your surgical team regarding showering and dressing changes.
- Report Any Concerns Immediately: If you develop a fever, or notice any pus, spreading redness, heat, or increased pain near the wound, contact your doctor or the surgical ward without delay.
By taking on this role, you are not being difficult; you are being a responsible and crucial member of your own healthcare team, extending the discipline of the operating room into your recovery space.
When to Change Your Dressing: The 3 Signs of Early Infection
One of the most common questions patients have is about their dressing. “Should I change it?” “Is this what it’s supposed to look like?” Your surgical team will give you specific instructions, and in most cases, the initial sterile dressing applied in the OR should be left untouched for a designated period. Its job is to protect the wound while it begins to heal. Changing it too early or unnecessarily can break that sterile seal and introduce bacteria. According to CDC clinical definitions, most surgical site infections will become apparent within 30 days of the procedure (or up to 90 days if an implant was placed), so this is the key window for vigilance.
Instead of worrying about the dressing itself, your focus should be on recognizing the early warning signs of a potential infection. Knowing what to look for transforms passive anxiety into active monitoring. There are three cardinal signs that should prompt you to contact your healthcare provider immediately:
Conceptually, as shown above, you are looking for changes in temperature, appearance, and sensation. Specifically, watch for:
- Increasing Redness and Warmth: Some redness around an incision is normal, but if it begins to spread outwards (like a red halo) or the area feels increasingly warm to the touch compared to the surrounding skin, it’s a red flag.
- Abnormal Drainage or Pus: A small amount of clear or slightly blood-tinged fluid can be normal in the first day or two. However, any thick, cloudy, yellow, or green drainage (pus), especially if it has a foul odor, is a clear sign of infection.
- Escalating Pain or Tenderness: Post-operative pain should gradually decrease. If the pain at the wound site suddenly gets worse, becomes a throbbing pain, or is extremely tender to a light touch, it needs to be assessed.
Recognizing these signs early is the most important thing you can do to ensure a small problem is treated quickly before it becomes a large one.
The Ward Hygiene Mistake That Undermines a Perfect Operation
A surgical procedure can be executed with flawless precision in the hyper-controlled environment of the OR, but that safety can be compromised if the same level of discipline is not carried over to the recovery ward. The single biggest “mistake” is a collective drop in vigilance—the assumption that because the surgery is over, the greatest risk has passed. In reality, the post-operative period is just as critical. The journey from the OR to the ward involves a transition from a near-sterile space to a general hospital environment with more people, more movement, and more potential sources of contamination.
This is where hospital-wide protocols become essential. It’s not about one person’s error, but about the integrity of the entire system. This includes: consistent hand hygiene from every single person who enters your room (doctors, nurses, technicians, cleaners, visitors), meticulous cleaning of high-touch surfaces like bed rails and call buttons, and ensuring any shared equipment is decontaminated between patients. The chain of defense built in the OR must be diligently maintained.
The good news is that a systematic focus on these measures works. These are not just hopeful theories; they are evidence-based practices that have a measurable impact on patient safety. This commitment to system-wide hygiene and infection control protocols is a major reason why hospitals have been able to make significant progress in patient safety. While the fight against superbugs is ongoing, these coordinated efforts are our most powerful weapon in the post-operative phase.
Why Must “Sterile” Instruments Undergo 121°C Steam for 15 Minutes Specifically?
We’ve talked about the sterile field and sterile dressings, but the concept of “sterility” for surgical instruments is on another level entirely. It is not a vague term; it is an absolute, scientifically-defined state. This is achieved through a process called autoclaving—sterilization using high-pressure, saturated steam. The specific standard of 121°C (250°F) for a minimum of 15 minutes is not arbitrary. It is the validated time and temperature required to kill the most resilient life forms on earth: bacterial spores.
Regular bacteria are relatively easy to kill. But some bacteria can form a dormant, armor-plated version of themselves called a spore, which can survive boiling water and harsh chemicals. The combination of intense heat and pressure inside an autoclave is designed to penetrate these defenses and ensure complete destruction, achieving what we call “Validated Sterility.” This means we have scientific proof that the process eliminates all microorganisms.
The reason for this uncompromising standard is the presence of foreign material in the body, such as a prosthetic joint, a pacemaker, or even stitches. Under normal circumstances, your immune system can handle a small number of bacteria. However, the WHO surgical safety guidelines specify that the risk of infection increases dramatically with more than 100,000 microorganisms per gram of tissue. Crucially, when a foreign body is present, that threshold for infection plummets to as few as 100 bacteria. We don’t aim to reduce the bioburden on instruments; we aim to eliminate it entirely, because the margin for error is virtually zero.
Key takeaways
- Prevention Is a System: Your safety relies on a multi-layered system of interconnected protocols, where each step is designed to break the chain of infection.
- You Are an Active Partner: From pre-op showering to post-op wound protection, your informed participation is a critical and empowering part of the safety process.
- Sterility Is Not Negotiable: In the operating theatre, “sterile” is a scientifically validated, absolute state achieved through rigorous, evidence-based processes that leave no room for error.
Why Do Surgical Instruments Cost Thousands When Similar Tools Are So Cheap?
At first glance, a pair of surgical forceps might look similar to a tool you could buy at a hardware store for a fraction of the price. This raises a logical question: why the enormous cost difference? The answer is the final, crucial piece of the infection prevention puzzle and directly relates to the harsh sterilization process we just discussed. The cost is not about appearance; it’s about material science and the absolute necessity of withstanding repeated, extreme sterilization cycles without fail.
A standard tool from a hardware store is made of ordinary steel. If you were to put it through a 121°C high-pressure steam autoclave cycle just once, it would likely begin to rust or corrode. If you did it hundreds of times, it would degrade, potentially flaking off microscopic metal fragments or leaching harmful elements. This is unacceptable in surgery. Surgical instruments are precision-engineered from specific, non-corrosive, and biocompatible materials. As experts from the National Institutes of Health note:
Surgical instruments are made from specific, non-corrosive, biocompatible alloys (like 316L surgical steel) that can withstand hundreds of high-pressure, high-temperature sterilization cycles without degrading, rusting, or leaching harmful metals into the body.
– PMC – Surgical site infections: a comprehensive review, Surgical site infection review
This resilience is non-negotiable. The instrument must be able to achieve Validated Sterility every single time it is used, for years on end, without its own material integrity becoming a risk to the patient. The high cost reflects the advanced metallurgy, precision manufacturing, and rigorous quality control required to produce a tool that is unconditionally safe for use inside the human body. It’s a perfect example of how every single detail in the surgical environment is optimized for one thing: your safety.
Armed with this knowledge, you are no longer just a passive patient but an informed participant. You can now have a more confident and meaningful discussion with your surgical team about the specific protocols they have in place for your procedure. Ask them questions. Understanding their process is the best way to build confidence and partner with them for the safest possible outcome.